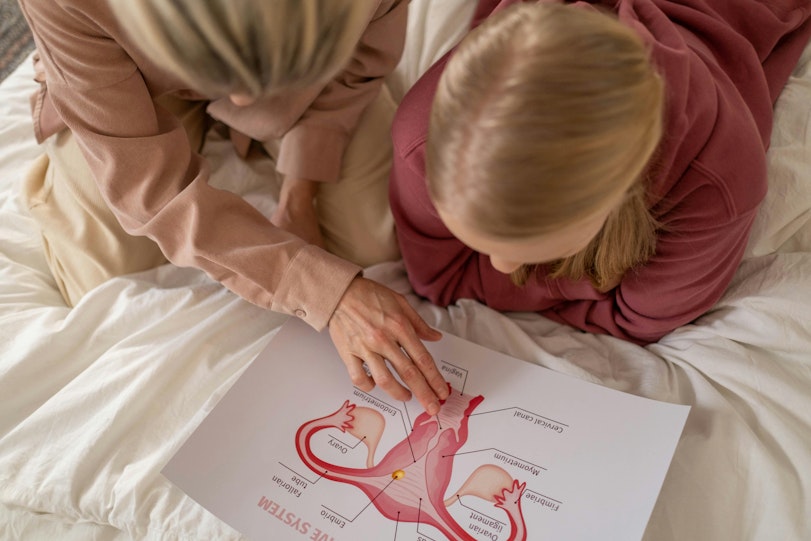
What is PMOS, the new name for PCOS?
Why PCOS just got a new name
Updated May 12, 2026
In this article
- In short
- Why has PCOS been renamed to PMOS?
- What does PMOS actually stand for?
- How common is PMOS in teen girls?
- What are the signs of PMOS in my daughter?
- When should I take my daughter to the doctor?
- How is PMOS diagnosed in teens?
- What can my daughter do to manage PMOS?
- How can I support my daughter emotionally?
- FAQ
- What's the best first step if I think my daughter has PMOS?
In short
Polycystic ovary syndrome (PCOS) has been officially renamed polyendocrine metabolic ovarian syndrome (PMOS) after a 14-year global review led by Monash University and published in The Lancet in May 2026.
The new name reflects what doctors have long known: PMOS is a whole-body hormone condition, not just an ovary problem.
It affects around 1 in 8 women, often starts in the teen years, and is very manageable with the right support.

Why has PCOS been renamed to PMOS?
Because the old name was misleading. PCOS made the condition sound like it was only about cysts on the ovaries, when in reality it affects hormones, metabolism, mood, skin, and weight across the whole body.
The change was announced at the European Congress of Endocrinology in Prague and published in The Lancet on 12 May 2026. It followed 14 years of work involving 56 medical and patient groups across six continents, led by Prof Helena Teede at Monash University.
Patients pushed hard for the change. Many had spent years feeling confused by a name that didn't match their symptoms or, in some cases, didn't match their bodies at all.
The “cyst” word in the original name refers to fluid-filled sacs, and not actual cysts.
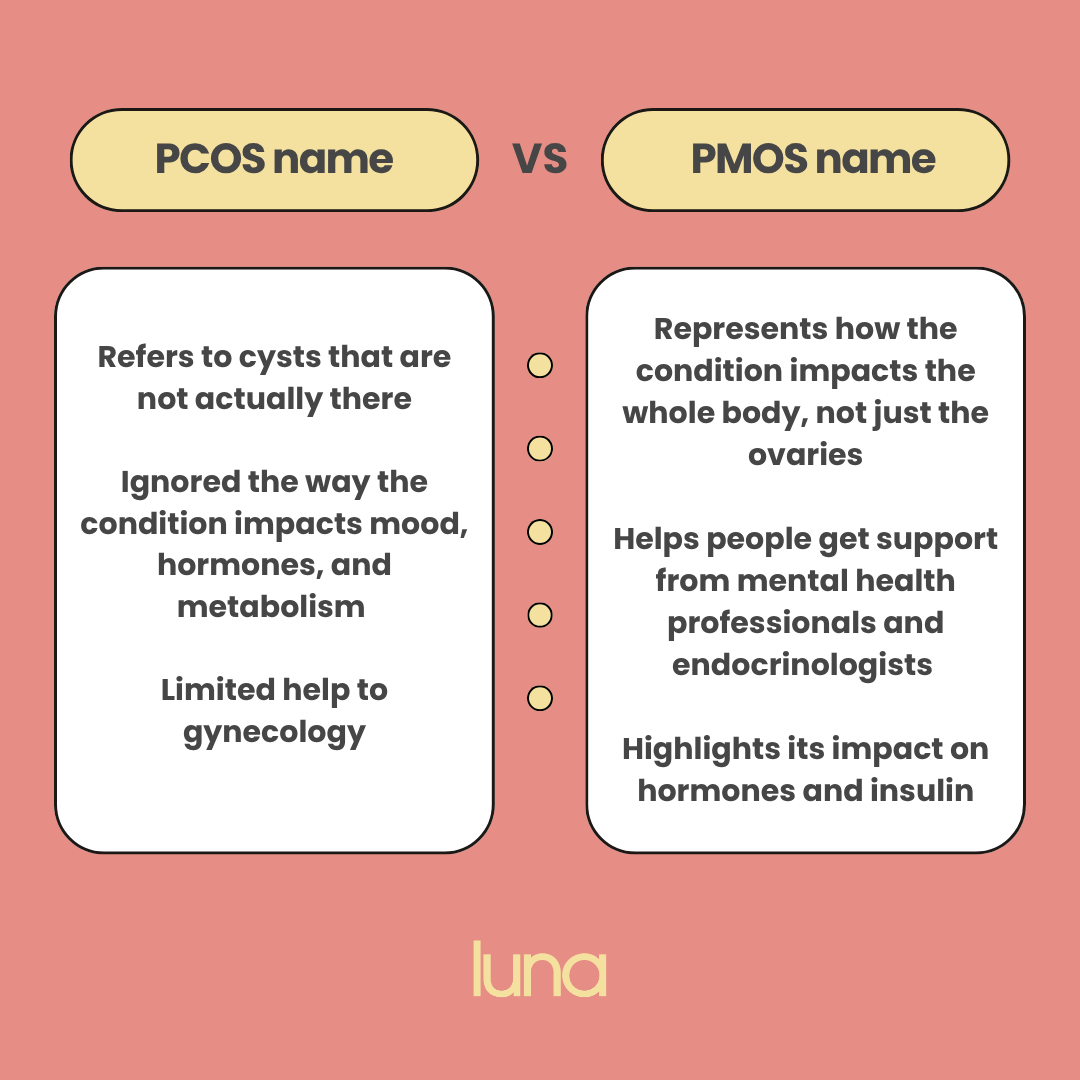
What does PMOS actually stand for?
PMOS stands for polyendocrine metabolic ovarian syndrome. Each word does a job:
- Polyendocrine: it affects multiple hormone systems, not just one
- Metabolic: it changes how the body handles insulin, sugar, and weight
- Ovarian: the ovaries are still involved, just not the whole story
- Syndrome: a cluster of symptoms that show up together
The shift matters because the old name pointed parents and patients toward gynaecologists, when many women with PMOS also need support from endocrinologists, doctors, dermatologists, and mental health professionals.

How common is PMOS in teen girls?
PMOS affects around 1 in 8 women worldwide, or roughly 170 million people. Symptoms often appear during puberty, which is why so many girls are diagnosed in their teens.
That said, PMOS is genuinely tricky to spot in teenagers, because some of its signs (irregular periods, acne, mood swings) can also just be a normal part of puberty settling down.
In a luna poll of 1,605 teen girls, only 13% said their periods were regular straight away, and most took a year or two to find a rhythm.
So one irregular period or a breakout doesn't mean PMOS. It's the pattern, over time, that matters.
What are the signs of PMOS in my daughter?
The most common signs of PMOS cluster around hormones, periods, and skin.
Keep an eye out for:
- Irregular or missing periods that don't settle into a rhythm 2 to 3 years after her first period
- Acne, especially on the jawline, chin, and back, that doesn't respond to normal skincare
- Excess hair growth on the face, chest, stomach, or back (called hirsutism)
- Thinning hair on the scalp
- Unexplained weight gain, particularly around the middle, or difficulty losing weight
- Fatigue, low mood, or anxiety that feels out of proportion
If you're noticing two or more of these, and they've been going on for a while, it's worth a chat with your doctor.
When should I take my daughter to the doctor?
If her periods are still very irregular more than 2 years after her first one, or if she's experiencing several PMOS symptoms together, book an appointment. You don't need to wait for things to feel "serious enough."
Doctors see this often, and there's no awkward exam involved for the first visit. The doctor will usually ask about her cycle, her skin, her weight, and her family history (PMOS often runs in families).
They may then suggest blood tests to check hormone levels, including testosterone, and do a scan of the ovaries.
If your daughter is anxious about going, it can help to remind her that the doctor has heard it all before, and that getting answers can be a huge relief.
Many girls describe feeling validated after a diagnosis: it explains things they'd been quietly worrying about for years.
How is PMOS diagnosed in teens?
PMOS is diagnosed using a mix of symptoms, blood tests, and sometimes an ultrasound. For teenagers, doctors are deliberately more cautious than they are with adults.
In adults, the Rotterdam criteria require two of three signs: irregular ovulation, high androgens (male-pattern hormones), and polycystic-looking ovaries on ultrasound.
But in teens, ovaries normally look "polycystic" on ultrasound during puberty, so most specialists no longer use ultrasound to diagnose PMOS in girls under 18.
Instead, diagnosis in teens usually relies on:
- Clear, persistent irregular periods after the first 2 to 3 years post-menarche
- Evidence of high androgens, either through symptoms (acne, hirsutism) or blood tests
- Ruling out other conditions like thyroid problems, which can look similar
Some doctors may want to "watch and wait" for a couple of years, especially if your daughter is newly menstruating.
That's normal practice, not dismissiveness, but you can always push for a referral to a paediatric endocrinologist if symptoms are affecting her daily life.
What can my daughter do to manage PMOS?
The most evidence-backed first step for managing PMOS is lifestyle support: healthy eating, regular movement and exercise she actually enjoys, good sleep, and stress management.
This isn't about weight loss or restriction. It's about giving her body steadier blood sugar and hormone levels.
If lifestyle isn't enough, doctors may prescribe:
- The combined contraceptive pill, to regulate periods and manage acne and hair growth
- Topical treatments for acne, or hair-reduction options for hirsutism
It's worth knowing that PMOS does not mean she won't be able to have children. Most women with PMOS can and do get pregnant, sometimes with a bit of help.
Old messaging around infertility caused a generation of teenagers unnecessary heartbreak, and the new guidelines push back firmly against it.
How can I support my daughter emotionally?
PMOS can quietly chip away at confidence. The symptoms (acne, weight, hair, mood) hit exactly the parts of life that already feel high-stakes in your teens. A diagnosis can land hard, especially if a doctor mentions fertility in passing.
You don't need to fix it. You just need to be the steady one. A few things that help:
- Acknowledge what she's feeling before jumping into solutions
- Let her lead how much she wants to talk about it
- Avoid commenting on her body, even kindly, while she's processing
- Help her find good information rather than late-night Googling alone
In a luna poll of 2,446 teen girls, more turned to Google or TikTok (31%) for health and wellbeing help than to doctors (2%), and only 1 in 4 (27%) went to a parent first.
Being one of the people she trusts to ask matters more than having all the answers.
If her mood feels stuck, talk to your doctor about mental health support alongside the PMOS care plan and explore free mental health resources.
FAQ
What's the difference between PCOS and PMOS?
There's no medical difference. PMOS is the new name for the same condition.
The change is about better describing what's already known: that the condition affects multiple hormone systems and metabolism, not just the ovaries.
If your daughter has a PCOS diagnosis, it's still valid, and her treatment won't change.
Can teenagers actually be diagnosed with PMOS?
Yes, but doctors are careful. Some signs of PMOS overlap with normal puberty, so doctors often wait until your daughter has been having periods for 2 to 3 years before confirming a diagnosis.
In the meantime, they can still treat individual symptoms like acne or painful periods.
Are PMOS and ovarian cysts the same thing?
No. The "cysts" referred to in the old name PCOS are actually small follicles holding immature eggs, not the kind of ovarian cysts that need surgery.
The renaming to PMOS partly aims to clear up exactly this confusion.
Will my daughter still be able to have children if she has PMOS?
In most cases, yes. PMOS can make ovulation irregular, but the vast majority of women with PMOS go on to have children, often without needing fertility treatment.
Managing PMOS well in the teen years is one of the best things she can do for her future fertility.
Does PMOS go away?
PMOS is a long-term condition, but symptoms can change a lot over the years and respond well to treatment.
What's the best first step if I think my daughter has PMOS?
The best first step is usually just tracking her period and her symptoms for a couple of months, so you've got something concrete to take to the doctor.
luna's period tracker is built specifically for tweens and teens, with no scary fertility prompts or adult content, and it makes the doctor conversation a lot easier.

How we created this article:
luna's team of experts comprises GPs, Dermatologists, Safeguarding Leads and Junior Doctors as well as Medical Students with specialised interests in paediatric care, mental health and gynaecology. All articles are created by experts, and reviewed by a member of luna's senior review team.
Sources:
The Lancet "Polyendocrine metabolic ovarian syndrome, the new name for polycystic ovary syndrome: a multistep global consensus process" | Accessed 12 May 2026
https://www.thelancet.com/journals/lancet/article/PIIS0140-6736%2826%2900717-8/fulltextThe Guardian "'Unprecedented' global effort gives new name to polycystic ovary syndrome" | Accessed 12 May 2026
https://www.theguardian.com/society/ng-interactive/2026/may/12/polycystic-ovary-syndrome-pcos-new-name-polyendocrine-metabolic-ovarian-syndrome-pmosAch T, Gorchane A, Methnani J, et al. "Rethinking the Terminology: A Perspective on Renaming Polycystic Ovary Syndrome." Clinical Medicine Insights: Endocrinology and Diabetes, 2024 | Accessed 12 May 2026
https://pmc.ncbi.nlm.nih.gov/articles/PMC11528641/NHS. "Polycystic ovary syndrome" | Accessed 12 May 2026
https://www.nhs.uk/conditions/polycystic-ovary-syndrome-pcos/Monash Centre for Health Research and Implementation. "International PCOS Guideline" | Accessed 12 May 2026
https://www.monash.edu/medicine/mchri/pcos/guidelineAskPCOS. "PCOS and fertility" | Accessed 12 May 2026
https://www.askpcos.org/articles/pcos-and-fertility/NICE "How should I diagnose polycystic ovary syndrome?" | Accessed 12 May 2026
https://cks.nice.org.uk/topics/polycystic-ovary-syndrome/diagnosis/diagnosis/We'd love to keep in touch!
Sign up to our parent newsletter for emails on the latest teen trends, insights into our luna community and to keep up to date
By signing up, you are agreeing that we can use your email address to market to you. You can unsubscribe from marketing emails at any time by using the link in our emails. For more information, please review our privacy statement.